Tibialis Posterior Tendinopathy can interrupt your plans for exercise and sports participation. What is Tibialis Posterior Tendinopathy? What causes it? What are the common symptoms? How to you treat it and how long until Tibialis Posterior Tendinopathy gets better? Keep reading to answer all you Tibialis Posterior Tendinopathy questions.
If reading this article isn’t quite your style, check out this short video with Dr. Abbey Davidson (Osteopath) on Tibialis Posterior Tendinopathy:
What is Tibialis Posterior Tendinopathy?
 The tibialis posterior muscle is the most central or deep of the leg muscles. It runs along the back of the tibia (shin bone) and the fibula. This muscle stabilizes the lower leg and foot arch while also playing a role in inversion (twisting inwards) and plantar flexion (pointing) of the foot/ankle. The tibialis posterior muscle is commonly involved with shin splints or shin pain.
The tibialis posterior muscle is the most central or deep of the leg muscles. It runs along the back of the tibia (shin bone) and the fibula. This muscle stabilizes the lower leg and foot arch while also playing a role in inversion (twisting inwards) and plantar flexion (pointing) of the foot/ankle. The tibialis posterior muscle is commonly involved with shin splints or shin pain.
The tibialis posterior tendon tracks behind the medial malleolus (inside ankle) and inserts onto the under surface of the smaller foot bones (navicular, medial cuneiform, metatarsals, cuboid and calcaneus). The tibialis posterior tendon or posterior tibial tendon is commonly injured in runners.
Tendinopathy is a term used for any disease or injury of a tendon. This can mean tendonitis (acute inflammation), tendonosis (chronic inflammation) or paratenonitis (inflammation of the outer tendon layer). This is inclusive of both inflammatory and micro-tear type injuries.
Causes of Tibialis Posterior Tendinopathy:
 Tibialis Posterior tendinopathy is most commonly bought on after a period of over-use, overloading or over training. This leads to friction building up as the tibialis posterior tendon loops around the medial malleolus of the ankle. Repeated episodes of friction result in tendinopathy or injury to the tibialis posterior tendon.
Tibialis Posterior tendinopathy is most commonly bought on after a period of over-use, overloading or over training. This leads to friction building up as the tibialis posterior tendon loops around the medial malleolus of the ankle. Repeated episodes of friction result in tendinopathy or injury to the tibialis posterior tendon.
Other factors which can lead to injury of the posterior tibialis tendon include:
- Sudden changes or increases in training habits (e.g. spontaneous decision to train for marathon)
- Change in training surface (grass to concrete)
- Poor footwear (High heeled shoes, old/unsupportive runners)
- Flat feet/poor foot mechanics
- Lack of strength (around the hips, knees, ankle and/or feet)
- Poor ankle flexibility
- Poor knee/hip mechanics or stability (placing more stress on the ankle joint)
- Excessive weight/load (with training weights or overall body weight)
Prevention is always better than cure. Try and avoid poor footwear, sudden changes in training habits and listen to your physiotherapist/osteopath in regards to injury prevention.
Symptoms of Tibialis Posterior Tendinopathy:
Common signs and symptoms of a tibialis posterior tendinopathy include:
- Pain/tenderness on the inside of your ankle, arch or foot and/or up shin bone
- Pain present during or after running, jumping, walking or prolonged standing
- Swelling or redness on the inside of your ankle
- Flattened foot arch
- Pain or inability to perform calf/heel raise
If you are concerned you may be suffering from a tibialis posterior tendinopathy it is important to be assessed by your physiotherapist or osteopath. Early assessment and diagnosis can lead to better outcomes/recovery.
What you can do right now for Tibialis Posterior Tendinopathy?
 If you think you may be suffering from a tibialis posterior tendinopathy it is important to rest, massage the area, wear appropriate footwear, stretch and perform strengthening exercises.
If you think you may be suffering from a tibialis posterior tendinopathy it is important to rest, massage the area, wear appropriate footwear, stretch and perform strengthening exercises.
Resting doesn’t necessarily mean stopping all of your physical activity. It means toning down your existing training (frequency and intensity) and allowing sufficient periods between your training sessions. If you have just recently started training in a new way it may mean starting at a less intense pace and progressively increasing to avoid re-injury.
Self-massage through the tibialis posterior muscle (behind the shin bone) and cross friction massage across the tibialis posterior tendon can help provide some relief. By relaxing the muscle belly you reduce the tension on the tendon as it loops around the medial malleolus. Stimulating the tendon promotes blood flow and healing at the site. The cross friction technique can be tender so only apply for 10-20 seconds at a time.
Footwear plays a huge role in foot and ankle mechanics. High heeled shoe wearing requires constant activation of the tibialis posterior muscle. Avoid this kind of footwear where possible especially when feeling inflamed. Old or unsupportive runners/sports footwear can lead to extra pressure being placed on the tibialis posterior tendon. Replacing your footwear to something more appropriate (ask your health professional for more details) will complement your recovery and help in avoidance for re-injury.
Stretching the calf (gastrocnemius and soleus) muscles and the tibialis posterior muscle can help relax and lengthen the muscle fibres. Stretches should be held for a minimal of 30 seconds and repeated 2-3 times. Stretching should be performed to a point where a comfortable tension is felt and not pain. A tibialis posterior stretch is demonstrated in the video at the top of page.
Strengthening exercises which focus on the calf and tibialis posterior muscles will for an important part of recovery from tibialis posterior tendinopathy. Adding strength and stability to the ankle and foot will lead to decreased force being placed on the tendon itself. The video at the top of page demonstrates some of these exercises.
Physio and osteo treatment for Tibialis Posterior Tendinopathy:
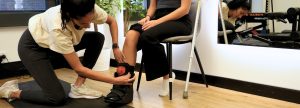
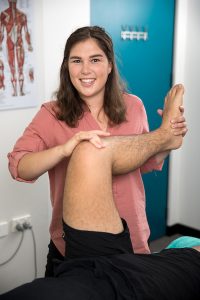 The first goal of visiting your physiotherapist or osteopath will be to establish what is causing your pain and other symptoms. They will ask you a bunch of relevant questions, assess range of motion at the ankle and surrounding joints and run specific orthopedic tests to narrow down the conditions you could be suffering. This in clinic assessment will usally provide enough information to diagnose you with a tibialis posterior tendinopathy but on some instances you may also be sent for imaging (ultrasound or MRI) to confirm.
The first goal of visiting your physiotherapist or osteopath will be to establish what is causing your pain and other symptoms. They will ask you a bunch of relevant questions, assess range of motion at the ankle and surrounding joints and run specific orthopedic tests to narrow down the conditions you could be suffering. This in clinic assessment will usally provide enough information to diagnose you with a tibialis posterior tendinopathy but on some instances you may also be sent for imaging (ultrasound or MRI) to confirm.
Your osteopath or physiotherapist will then spend time educating you about your condition and how both you and your practitioner will contribute to the management of your condition until resolution. This may also include advice on how to avoid re-injury or preventing injures of a similar nature in the future.
Hands on therapy will include improving the mechanics on the entire lower limb (including hip, knee, ankle and foot), decreasing muscular tension, improving joint range of motion/flexibility and increasing blood flow to the affected tendon. In addition you will be prescribed a range of at-home exercises to perform which will help in your recovery and future injury prevention outside of the clinic. Your physio or osteo will also over-see your return to sport to minimize your chance of re-injury.
How long until Tibialis Posterior Tendinopathy gets better?
How fast you recover from an posterior tibialis tendinopathy will vary depending on the specific cause, your compliance to management protocol and how long your symptoms have been present. Generally, a tendinopathy will respond to conservative management with your physiotherapist or osteopath within 4-6 weeks.
If symptoms are present for more than 6 months’ of conservative management alternate therapies may be considered. This may involve Steroid injections, PRP injections or surgery.
Untreated posterior tibialis tendinopathy can result in tendon rupture.
By Sydney CBD Osteopath Dr Abbey Davidson